The question is no longer whether scientists can justify pursuing longer, healthier lives. Instead, the burden now falls on defenders of forced ageing to explain why needless suffering should persist. The Ethics Case for Longevity Science Zhuang Zhuang Han, João Pedro de Magalhães.
This month’s theme: GLP-1, first coumpound with broad positive effects for longevity?
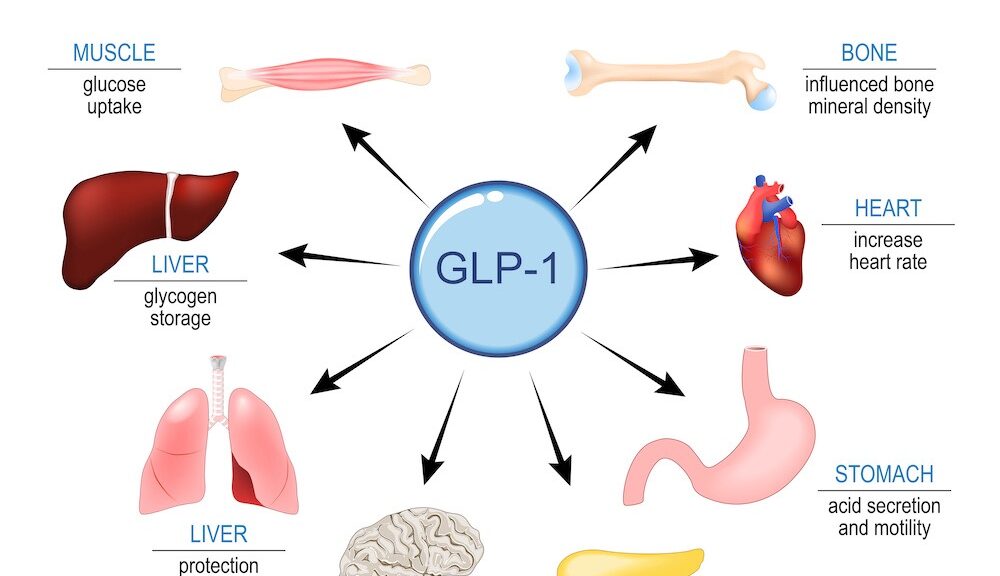
GLP-1 (glucagon-like peptide-1) is a hormone naturally produced in the intestines that helps regulate blood sugar levels, digestion, and appetite. It works by stimulating the pancreas to release insulin when blood sugar is high, while also reducing the release of glucagon, a hormone that raises blood sugar. Additionally, GLP-1 slows the rate at which food leaves the stomach, which helps prevent sudden spikes in blood sugar after eating and promotes a feeling of fullness. Medications that mimic GLP-1 are commonly used to treat type 2 diabetes and support weight management, and they are also being studied for potential benefits in heart health and metabolic aging.
GLP-1 receptor agonists (GLP-1RAs) act far beyond glucose control, intersecting with several hallmarks of aging. They reduce chronic low-grade inflammation by lowering CRP and pro-inflammatory cytokines, improve insulin/IGF-1 signaling, enhance mitochondrial efficiency, and decrease oxidative stress. Preclinical studies show improved mitochondrial biogenesis and reduced cellular senescence markers in metabolic tissues. These pathways are central to geroscience because dysregulated nutrient sensing, mitochondrial dysfunction, and inflammaging drive multiple age-related diseases. By restoring metabolic flexibility and reducing lipotoxicity, GLP-1 therapies may function as metabolic reprogrammers, shifting physiology toward a lower biological age phenotype.
Obesity trends and public health
In the United States, adult obesity prevalence climbed almost continuously from the late 1970s through the 2010s, driven by an obesogenic food environment, sedentary lifestyles, and widening socioeconomic disparities. National Health and Nutrition Examination Survey (NHANES) data showed rates rising from roughly 30% in 1999–2000 to over 42% by 2017–2020, with severe obesity increasing even faster. However, the most recent national surveillance reports (2021–2023) suggest a possible plateau, and in certain age and income subgroups, a slight decline, occurring alongside the rapid adoption of GLP-1 receptor agonists for both diabetes and obesity treatment. Pharmacy and claims data indicate several-fold growth in prescriptions for semaglutide and tirzepatide during this period, with the highest uptake among middle-aged adults and those with private insurance.
Large outcome trials demonstrate that GLP-1RAs reduce major adverse cardiovascular events (MACE), even in non-diabetic individuals with obesity. The SELECT trial showed a 20% reduction in MACE with semaglutide in people with overweight/obesity and established CVD. In parallel, GLP-1 therapies improve non-alcoholic fatty liver disease (NAFLD/NASH) through weight-independent mechanisms, including reduced hepatic steatosis and inflammation. Benefits also extend to blood pressure, lipid profiles, and heart failure symptoms, suggesting multi-system healthspan effects rather than single-disease treatment.-
Fat loss vs. muscle preservation
While GLP-1 drugs produce substantial weight loss (≈10–15% with semaglutide), up to 25–40% of total weight lost can be lean mass if no countermeasures are taken. For longevity, preserving skeletal muscle is critical to avoid sarcopenia and frailty. Clinical guidance increasingly emphasizes high protein intake, resistance training, and progressive loading during GLP-1 therapy. Emerging data suggest that combining GLP-1 with structured exercise improves fat-to-lean loss ratio and functional outcomes, aligning weight reduction with healthspan goals rather than simple mass reduction.
Combination Longevity Therapies
GLP-1 drugs seem to generate largely positive effects, but are unlikely to be standalone gerotherapeutics but may serve as foundational metabolic platforms. Combining GLP-1 with exercise enhances mitochondrial function and cardiorespiratory fitness; pairing with metformin targets complementary nutrient-sensing pathways; future combinations with rapalogs or senolytics could address multiple hallmarks simultaneously. The geroscience model favors such stacked interventions to achieve additive or synergistic effects on healthspan and disease prevention. Clinical trials exploring multi-modal metabolic and anti-aging strategies are now a key frontier.
Semaglutide, liraglutide, dulaglutide, exenatide, albiglutide, and lixisenatide are all medications in the GLP-1 receptor agonist class, which are primarily used to improve blood sugar control in people with type 2 diabetes and, in some cases, to support chronic weight management. Across this medication class, common side effects include nausea, reduced appetite, and slowed stomach emptying, and all require medical supervision to ensure proper dosing and safety monitoring.
Commonly Prescribed GLP-1 Medications
- Semaglutide is one of the newer and more potent options and is available as both a once-weekly injection and a daily oral tablet; it is widely recognized for producing significant weight loss and cardiovascular benefits in addition to glucose control.
- Liraglutide is an older GLP-1 medication given as a daily injection and has an extensive safety record, although it typically results in slightly less weight loss than semaglutide.
- Dulaglutide is administered as a once-weekly injection and is popular because of its user-friendly auto-injector device and strong evidence for cardiovascular risk reduction, though its weight-loss effect is generally moderate.
- Exenatide was one of the earliest GLP-1 receptor agonists and is available as either a twice-daily injection or a once-weekly extended-release formulation; it remains effective for blood sugar management but is often considered less potent for weight reduction than newer medications.
- Albiglutide is another once-weekly GLP-1 agent that was previously used for diabetes treatment but has been withdrawn from many markets and is no longer commonly prescribed.
- Lixisenatide is a daily injection mainly used for type 2 diabetes, particularly effective at controlling blood sugar spikes after meals, although it generally produces less weight loss than newer GLP-1 drugs.
This is the first drug to have potentially such a large positive effect in the majority of the population in the USA. However, it is because this population is overweight or obese. We also still have to see impact in the long term since the drugs are recent. Still, we have a global positive effect on healthy longevity.
The good news of the month- Latest pancreatic cancer research shows potential to shrink and eliminate tumors
A research team led by Mariano Barbacid at the Spanish National Cancer Research Centre (CNIO) has developed an experimental triple-combination therapy that completely eliminated pancreatic tumors in mice with no major side effects. The study, published in Proceedings of the National Academy of Sciences (PNAS), focuses on pancreatic ductal adenocarcinoma (PDAC), a highly aggressive cancer with a very low five-year survival rate.
The therapy works by blocking three points in the KRAS signaling pathway, a gene mutation present in about 90% of pancreatic cancer cases. By targeting multiple points rather than a single one, the treatment prevented tumor resistance and produced long-lasting tumor regression in mouse models. The drug combination included an experimental KRAS inhibitor, an approved cancer drug, and a protein degrader. Although the results are very promising, researchers say more work is needed before clinical trials in humans can begin.
News of Heales and the Longevity Community
On Wednesday, April 8, there will be an international demonstration for funding longevity with people demonstrating in many cities. In Brussels, we will have a small gathering Place de la Monnaie from 17 to 18:00 CET. More information: fundlongevity.org/en/
For more information